What is healthcare automation?
Healthcare automation is the use of technology — including robotic process automation (RPA), artificial intelligence, and intelligent workflow software — to handle repetitive, rule-based administrative and clinical tasks without manual human input. It reduces errors, cuts operational costs, and frees clinical staff to focus on patient care instead of paperwork.
Ask any healthcare administrator what their biggest operational challenge is, and you will hear the same answer in different words.
Too much time on paperwork. Not enough time on patients.
The average physician spends nearly two hours on administrative tasks for every hour of direct patient care, according to research published in the Annals of Family Medicine. Nurses, practice managers, billing teams, and front desk staff face the same imbalance — consumed by data entry, insurance verification, appointment reminders, and claims processing that technology could handle automatically.
Healthcare automation closes that gap. Not by replacing clinical judgment — but by removing the administrative burden that sits between clinical staff and the work they were trained to do.
This guide covers what healthcare automation is, the types that deliver the strongest results, which processes benefit most, and how to evaluate whether your organization is ready to start.
What Is Healthcare Automation?
Healthcare automation is the application of software technology to perform administrative, operational, and clinical support tasks that currently require manual human effort. These include scheduling appointments, verifying insurance eligibility, processing claims, sending patient reminders, routing referrals, managing contracts, and generating compliance reports.
The key distinction is this: healthcare automation does not replace clinical decision-making. It replaces the repetitive, rule-based tasks that surround clinical work — the tasks that consume staff time, generate errors, and create friction for both patients and providers.
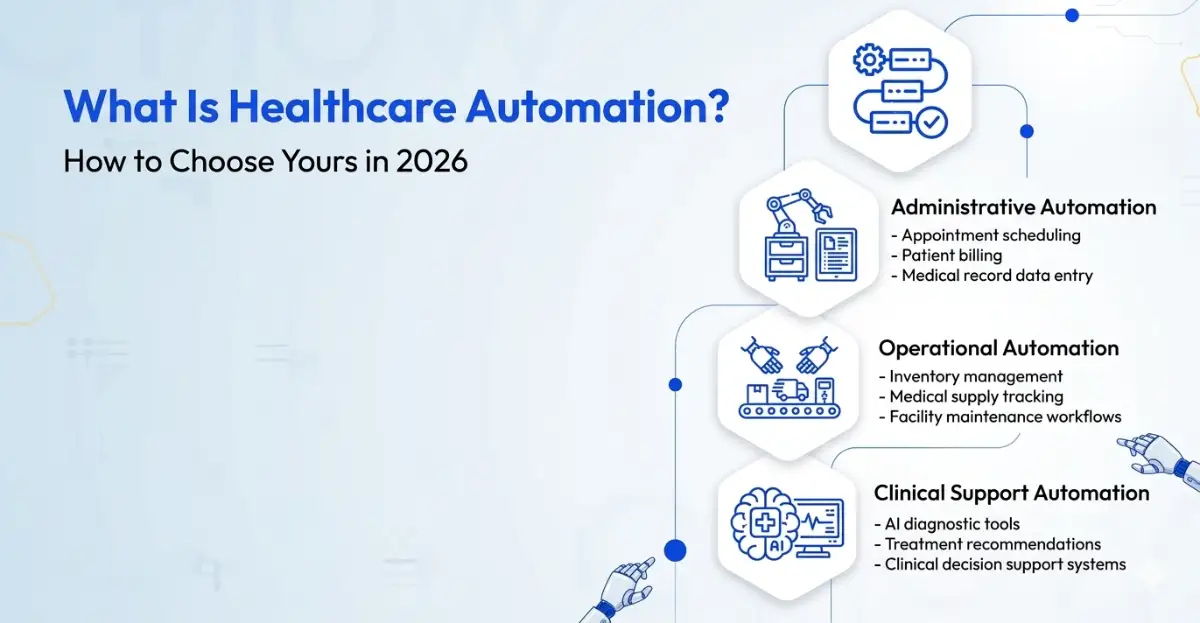
There are three layers at which automation operates in healthcare:
- Administrative automation — scheduling, registration, billing, claims, credentialing, and patient communication
- Operational automation — supply chain management, inventory tracking, contract management, reporting, and compliance documentation
- Clinical support automation — prior authorization, referral processing, EHR data entry, and care coordination workflows
Each layer delivers measurable time savings and error reduction independently. When combined into an integrated automation program, the cumulative impact on operational efficiency and patient experience is significant.
The purpose of automation in healthcare is to reduce the administrative burden on clinical and operational staff, eliminate manual errors in billing and documentation, accelerate patient-facing processes like scheduling and insurance verification, and free healthcare providers to spend more time on direct patient care rather than paperwork.
Types of Healthcare Automation
Understanding the different types of healthcare automation helps organizations match the right technology to the right problem — and avoid investing in solutions that are more complex than the use case requires.
Robotic Process Automation (RPA) in Healthcare
RPA deploys software bots that mimic human interactions with digital systems — logging into applications, extracting data, filling forms, moving files, and triggering workflows — without changing underlying infrastructure. In healthcare, RPA is the most widely deployed automation technology because it works with legacy EHR and billing systems that have no modern API.
Healthcare RPA handles tasks like insurance eligibility verification, claims status checking, prior authorization submission, patient data migration between systems, and regulatory reporting. It is fast to deploy, requires no system replacement, and typically delivers measurable ROI within 60–90 days. Our RPA development services guide covers the full scope of what RPA can automate and how to evaluate providers.
Intelligent Process Automation (IPA)
Intelligent process automation in healthcare extends RPA with AI capabilities — adding natural language processing, machine learning, and document understanding to handle unstructured data. Where RPA handles structured, predictable inputs, IPA can process medical records, clinical notes, insurance documents, and patient communications that do not follow a fixed format.
IPA is the right approach for healthcare organizations dealing with complex document-heavy workflows — prior authorization with clinical criteria, contract management automation, or claims that require contextual judgment rather than simple rule-following.
Workflow Automation
Healthcare workflow automation connects the systems and people involved in a process into a defined, triggered sequence. When a patient books an appointment, a workflow fires: confirmation sent, insurance verified, intake forms distributed, reminder triggered 48 hours before, follow-up scheduled post-visit. No staff member manages any of these steps manually.
Workflow automation in healthcare is built on platforms like n8n or integrated directly into CRM and practice management software. The defining characteristic is that processes move automatically based on triggers and conditions — not on someone remembering to do the next step.
Healthcare Marketing Automation
Healthcare marketing automation manages patient communication at scale — appointment reminders, recall campaigns, review requests, re-engagement sequences for lapsed patients, and post-visit follow-up — without requiring staff to manually send each message. Done correctly, healthcare marketing automation improves patient retention, increases appointment adherence, and generates significantly more online reviews without additional staff time.
AI-Powered Automation
AI and automation in healthcare combine large language models, computer vision, and predictive analytics with workflow execution. AI automation can triage inbound patient messages, summarize clinical documentation, predict no-show risk and trigger proactive outreach, and classify insurance claims for routing — capabilities that go significantly beyond what rule-based RPA can handle.
Benefits of Healthcare Automation
The business case for automation in the healthcare sector is well-established. Here is what consistently shows up in production deployments:
- 40–70% reduction in time spent on administrative tasks for targeted workflows
- Near-zero error rates on structured data processes versus a 2–5% human error baseline in manual data entry
- Faster claims processing — automated claims submission and status tracking reduces denial rates and accelerates reimbursement cycles
- Improved patient experience — automated reminders, faster intake, and consistent follow-up directly improve patient satisfaction scores
- Regulatory compliance — automated audit trails and documentation ensure every process step is recorded, reducing compliance risk in HIPAA-regulated environments
- Staff redeployment — clinical and administrative staff redirected from repetitive tasks to higher-value patient interaction and care coordination
- Scalability without headcount — automation scales with patient volume without proportional increases in administrative staff
According to McKinsey’s healthcare research, up to 30% of healthcare tasks could be fully automated with current technology — with the highest concentration in administrative and operational functions.
Healthcare Automation Use Cases by Department
Front office and patient access
- Patient scheduling — online booking systems connected to practice management software automatically fill appointment slots, send confirmations, and manage cancellation and rebooking sequences
- Insurance eligibility verification — RPA bots check coverage in real time against payer systems before each appointment, eliminating manual phone calls and reducing claim denials from eligibility errors
- Patient intake forms — digital intake distributed automatically before appointments, responses imported directly into the EHR, reducing check-in time and eliminating paper-based transcription errors
- Appointment reminders — multi-channel reminder sequences (SMS, email, voice) reduce no-show rates by 20–40% in documented deployments
Revenue cycle and billing
- Claims submission — automated claims generation from EHR data and direct submission to payers, with error checking before submission to reduce initial denial rates
- Denial management — automated denial tracking, root cause categorization, and resubmission workflows that would otherwise require dedicated billing staff hours daily
- Payment posting — automated posting of ERA/EOB payments to patient accounts, reducing manual reconciliation from hours to minutes
- Accounts payable automation for healthcare — invoice processing, PO matching, and approval routing handled automatically, reducing AP processing costs by 40–60% in well-scoped implementations
Clinical operations
- Prior authorization — automated PA submission and status tracking for procedures requiring payer approval, reducing the administrative time that currently delays patient care
- Referral management — referral requests generated, sent, and tracked automatically with status updates to both the referring provider and patient
- EHR documentation support — AI-assisted clinical note generation and documentation automation that reduces physician time spent on EHR entry
Operations and compliance
- Healthcare supply chain automation — inventory monitoring, automated reorder triggers, and supplier communication that eliminates manual stock management
- Contract management automation — payer and vendor contract tracking with automated renewal alerts, compliance monitoring, and approval workflows
- Healthcare employment verification — automated credential verification and employment history checks for clinical staff onboarding, reducing credentialing timelines significantly
- Compliance reporting — automated generation of regulatory reports with full audit trails, reducing the manual compilation time that currently consumes compliance team capacity
RPA in Healthcare: What It Does and Where It Fits
Robotic process automation in the healthcare industry is the most mature and widely deployed automation technology for administrative workflows. Its key advantage is that it works at the user interface level — meaning it can interact with legacy systems that have no API and no integration capability.
For healthcare organizations running older EHR platforms, billing systems, or payer portals, RPA is frequently the only practical automation option that does not require expensive system replacement. A hospital RPA bot can log into a payer portal, check prior authorization status, and update the internal system — tasks that currently consume multiple staff hours daily — without any changes to the underlying systems on either side.
The most impactful RPA use cases in the healthcare industry are insurance eligibility verification, prior authorization, claims status checking, patient data migration, and regulatory reporting — all high-volume, rule-based processes with consistent inputs that RPA handles reliably at scale.
| Healthcare process | Automation type | Typical time saving | Primary benefit |
|---|---|---|---|
| Insurance eligibility verification | RPA | 85–95% | Eliminates manual payer portal checks |
| Prior authorization | RPA + IPA | 60–75% | Faster approvals, fewer delays |
| Claims submission | RPA | 70–80% | Lower denial rates, faster payment |
| Appointment reminders | Workflow automation | 95–100% | 20–40% no-show reduction |
| AP invoice processing | RPA + IPA | 60–70% | Faster payment cycles, audit trail |
| Patient intake | Workflow automation | 80–90% | Faster check-in, fewer data errors |
| Compliance reporting | RPA | 70–85% | Consistent, auditable documentation |
AI and Automation in Healthcare in 2026
The combination of AI and automation in healthcare has moved significantly beyond proof-of-concept in 2026. Healthcare organizations are deploying AI-powered automation for three categories of work that rule-based RPA cannot handle:
Unstructured document processing — clinical notes, medical records, insurance documents, and prior authorization letters contain information that does not follow a predictable structure. AI models extract, classify, and route this information automatically, replacing manual review by billing staff, coders, and care coordinators.
Intelligent patient communication — AI triage systems classify inbound patient messages by urgency and intent, route them to the appropriate clinical or administrative team, and in many cases respond autonomously to routine enquiries — appointment availability, prescription refill status, test results communication — without clinical staff involvement.
Predictive operational workflows — AI models predict no-show probability for scheduled appointments and trigger proactive outreach to at-risk patients. They predict claim denial likelihood before submission and flag issues for correction. They monitor supply inventory patterns and optimize reorder timing. These are not reactive automations — they are proactive systems that prevent problems before they occur.
How to Start with Healthcare Workflow Automation
The most common mistake healthcare organizations make when starting their automation journey is trying to automate everything at once. The organizations that see the strongest early ROI start narrow and expand systematically.
Here is the right approach:
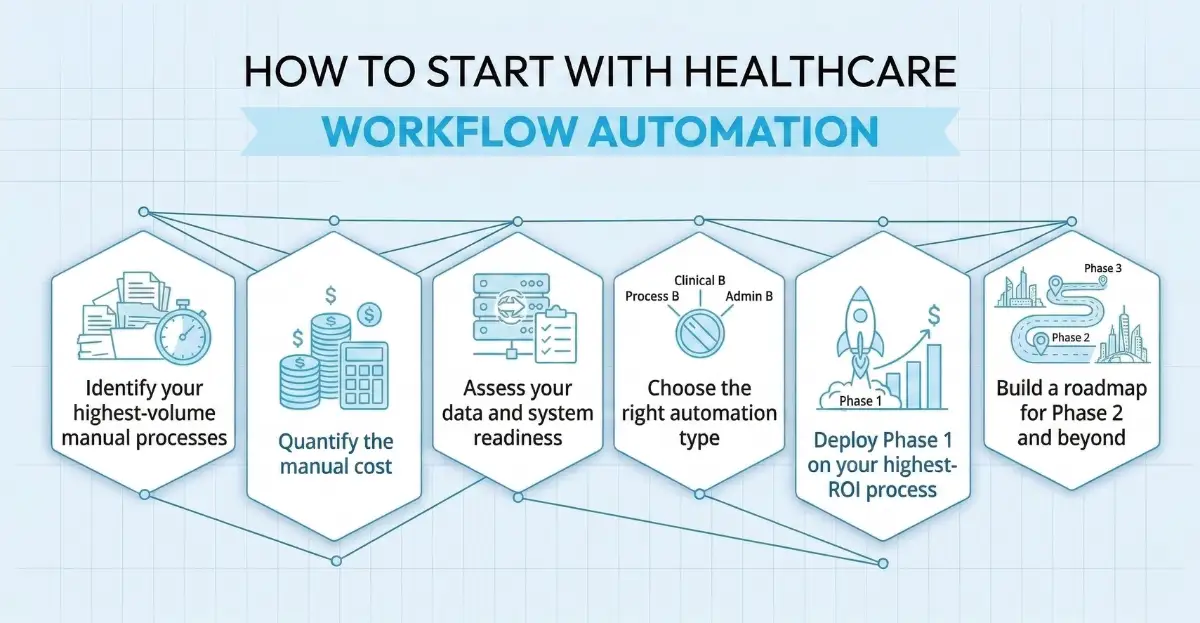
- Identify your highest-volume manual processes — the tasks your team performs most frequently that follow consistent, predictable steps. Insurance eligibility verification and appointment reminders are almost always the right starting point.
- Quantify the manual cost — calculate how many staff hours per week the process consumes, multiply by 50 working weeks, and multiply by average staff cost. That is your automation ROI baseline.
- Assess your data and system readiness — automation quality depends on data quality. Identify which systems the process touches and whether they have APIs, or whether RPA at the UI level is required.
- Choose the right automation type — structured, predictable inputs → RPA. Document-heavy with variable formats → IPA. Multi-step cross-system workflows → workflow automation. Patient communication at scale → marketing automation + AI.
- Deploy Phase 1 on your highest-ROI process — validate results, measure time savings, and build organizational confidence before expanding the automation program.
- Build a roadmap for Phase 2 and beyond — a single automation generates efficiency gains. A connected automation program — where patient scheduling, eligibility verification, intake, reminders, claims, and follow-up all work as a system — generates transformational operational improvement.
For healthcare organizations that want to move from evaluation to deployment quickly — with the right architecture, HIPAA-compliant infrastructure, and a team that has built healthcare automation systems before — working with a specialist like Exotica AI Solutions compresses months of internal development into weeks of structured delivery.
Frequently Asked Questions
Healthcare automation is not a future investment. For most healthcare organizations in the US and Canada, it is an immediate operational priority — because the cost of not automating is already being paid in staff time, billing errors, denied claims, and patient experience gaps that compound every week.
The question is not whether to automate. It is which process to start with, which technology fits, and whether your organization has the internal capacity to deploy it correctly or needs a specialist partner to accelerate the path to results.
Start with your highest-volume manual process. Quantify the cost. Deploy Phase 1. Build from there.
Ready to identify your highest-value automation candidates? Talk to the Exotica AI Solutions team today.

Mohit Thakur is an experienced Digital Marketing Expert, SEO Team Leader, and Content Writer with over 6 years of expertise in search engine optimization, content strategy, and digital growth. He specializes in research-driven SEO and crafting high-quality, compelling content that helps businesses improve their online visibility, organic traffic, and lead generation.
With hands-on experience across multiple industries, Mohit focuses on creating user-focused, well-researched content aligned with the latest Google algorithms and AI search trends. His approach combines technical SEO, content writing, content optimization, and data analysis to deliver consistent and measurable results.