What is insurance automation?
Insurance automation
- uses AI, robotic process automation (RPA), and intelligent workflow software to handle repetitive, rule-based tasks across the insurance value chain — including claims processing, document validation, underwriting, eligibility verification, and policy administration — without requiring manual intervention at every step.
The result: faster cycles, lower costs, fewer errors, and better fraud detection.
The insurance industry has always been built on paperwork, manual reviews, and slow-moving processes. A single claims cycle once took weeks — adjusters reviewing documents by hand, underwriters running risk assessments manually, and customer service reps fielding the same eligibility questions hundreds of times a day. That era is ending fast.
Insurance automation refers to the use of software, AI, and robotic process automation to handle repetitive, rule-based tasks across the insurance value chain — without human intervention at every step. This is not just about replacing manual data entry. Modern insurance automation spans:
- Intelligent document processing — extracting structured data from forms, medical records, and policy applications automatically
- Automated underwriting decisions — scoring risk in near-real time using ML models and third-party data feeds
- Claims triage and adjudication — routing, validating, and paying straightforward claims without adjuster involvement
- Eligibility verification — checking patient coverage in real time without manual portal logins
- Fraud detection — cross-referencing claims data against behavioral and historical patterns at scale
- Policy administration — automating issuance, endorsements, renewals, and cancellations end-to-end
According to McKinsey & Company, up to 25% of insurance industry tasks could be fully automated with currently available technology. For many mid-size carriers, that translates directly into seven-figure cost reductions annually — before accounting for downstream improvements in customer retention and denial rates.
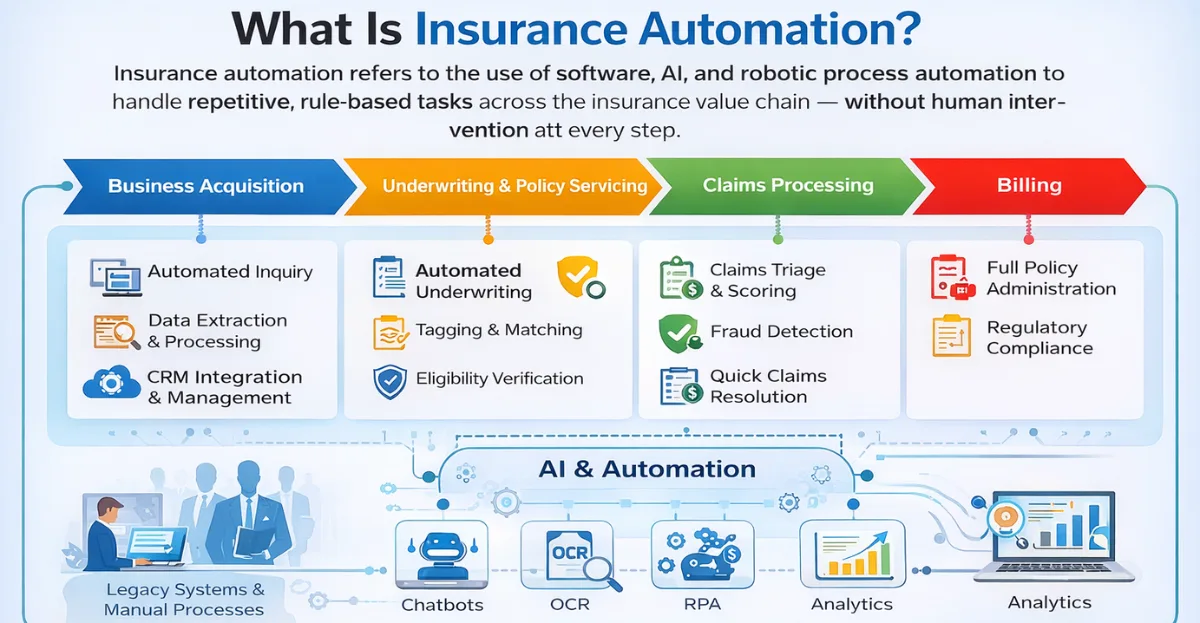
What Is Insurance Automation?
Insurance automation refers to the use of software, AI, and robotic process automation to handle repetitive, rule-based tasks across the insurance value chain — without human intervention at every step. This is not just about replacing manual data entry. Modern AI in insurance spans intelligent document processing, automated underwriting, claims triage, eligibility verification, fraud detection, and full policy administration.
Insurance carriers and agencies are not automating because it is trendy. They are doing it because the math has changed. Labor costs are rising. Customer expectations for faster claims resolution have hit all-time highs. Regulatory compliance requirements grow more complex each year. Meanwhile, legacy systems built for a paper-first world are creating operational bottlenecks that no amount of hiring can fix.
Three structural forces are accelerating adoption right now:
- Rising operating costs — manual claims handling costs 3–5x more per transaction than automated processing
- Payer mandate pressure — CMS and state regulators are shortening claims resolution timelines, making manual workflows legally risky
- AI maturity — large language models and document AI have finally reached the reliability threshold needed for production insurance workflows
Core Areas Where Automation Is Transforming Insurance
1. Automated Claims Processing
Claims handling is where automation delivers the most immediate, measurable impact. Automated insurance claims processing eliminates the manual touchpoints that create delays — intake, document validation, coverage verification, adjudication, and payment — and connects them into a continuous, rules-driven workflow automation pipeline.
- Straightforward claims — a clean medical bill or clear incident report can be handled end-to-end with zero human involvement
- Complex claims — routed to adjusters pre-sorted, pre-verified, and with key data already extracted
- Health insurance claims automation — especially high-value given high volume and strict regulatory timelines; see our full guide to healthcare AI solutions
- Cycle time improvement — drops from days to hours for clean claims, improving customer satisfaction scores directly
2. Insurance Document Automation
Insurance is one of the most document-intensive industries on earth. Policy applications, medical records, EOBs, proof of loss forms, inspection reports — the volume is staggering. Insurance document automation uses AI-powered extraction and Retrieval-Augmented Generation (RAG) to pull structured data from unstructured documents at scale.
- Document classification — automatically identifies document type on intake — claim form vs. medical record vs. EOB
- Data extraction — pulls named fields (dates, CPT codes, diagnosis codes, policy numbers) without manual keying
- Validation layer — cross-checks extracted data against existing policy records and flags discrepancies
- Intelligent routing — sends documents to the correct queue based on type, coverage line, or exception rules
3. Automated Insurance Underwriting
Underwriting automation applies machine learning models to risk assessment, replacing or augmenting the manual review process that has historically been the biggest bottleneck in the policy lifecycle. Automated insurance underwriting pulls from application data, third-party data sources, historical loss data, and predictive models to generate risk scores and coverage recommendations in near-real time. Our custom Python development team builds proprietary scoring models tailored to your specific book of business.
- Life and health carriers — underwriting automation can compress time-to-bind from days to minutes
- Commercial lines — frees underwriters to focus on complex, non-standard risks while automation handles the routine book
- Continuous improvement — risk scoring improves over time as more outcomes data accumulates through model retraining
4. Automated Insurance Verification
One of the highest-friction points in healthcare and benefits administration is eligibility verification. Automated insurance verification allows medical clinics, hospitals, and third-party administrators to check patient coverage in real time — without calling payer hotlines or manually logging into portals.
- Cloud-based tools — integrate directly with payer systems, returning eligibility data in seconds
- Front-desk impact — reduces workload significantly for high-volume medical clinics and intake teams; explore more in our guide to AI in healthcare
- Denial reduction — lowers claim denials from eligibility errors — one of the top five denial causes in US healthcare billing according to CMS
5. Insurance Workflow Automation and Policy Administration
How do insurance companies automate policy administration? Insurance workflow automation connects your CRM, policy administration system, document management, and communication tools into a single orchestrated process. When a customer requests a policy change, automation handles the verification, updates the record, generates updated documents, and sends the confirmation — without anyone touching a keyboard.
The five-step policy administration automation sequence:
- 01. Event trigger — renewal date reached, change request received, or payment event fires the workflow
- 02. Automated verification — system checks eligibility, coverage rules, and compliance requirements without manual lookup
- 03. Record update — policy administration system updated across all relevant fields with full audit trail preserved
- 04. Document generation — updated policy documents, ID cards, and confirmation letters generated automatically
- 05. Communication sent — policyholder notified via preferred channel; exceptions flagged to a human reviewer
Robotic Process Automation (RPA) in Insurance
RPA in insurance refers to software bots that replicate human interactions with existing software systems — logging into portals, copying data between systems, running scheduled reports, processing form submissions. Robotic process automation in insurance is especially valuable when you need to automate without replacing your core systems. For teams evaluating platforms, our comparison of n8n vs Zapier for hyperautomation is a useful starting point for selecting the right automation backbone.
Common robotic process automation insurance use cases:
- Extracting data from claims forms and entering it into legacy policy administration systems
- Running nightly eligibility batch checks against payer databases
- Generating compliance reports from multiple data sources on a scheduled basis
- Sending automated follow-up communications at defined workflow stages
- Flagging claims outside normal processing parameters for human adjuster review
- Syncing data between CRM, billing, and document management systems
RPA sits at the foundational layer of insurance automation — it is fast to deploy, delivers quick ROI, and does not require rebuilding your existing tech stack. Most insurance automation programs start with RPA bots on two or three high-volume processes and expand from there. According to Forrester Research, organizations with mature automation practices generate significantly more operational output at lower per-transaction cost than those still relying on manual processing.
Intelligent Automation in Insurance: The Next Layer
Where RPA handles structured, rule-based tasks, intelligent automation in insurance adds cognitive capability — the ability to handle variability, extract meaning from unstructured content, and make judgment-based decisions within defined parameters.
RPA vs. Intelligent Automation — Capability Comparison
| Capability | RPA | Intelligent Automation | Best For |
|---|---|---|---|
| Structured data tasks | Strong | Strong | Data entry, form processing |
| Unstructured documents | Limited | Strong | Medical records, inspection reports |
| Exception handling | Rule-based only | AI-driven | Complex or variable claims |
| Fraud detection | Pattern rules only | ML anomaly scoring | Claims validation, document fraud |
| Improves over time | No | Yes — continuous learning | Underwriting, fraud, triage |
Intelligent process automation in insurance combines RPA with AI capabilities: natural language processing for reading documents and communications, machine learning for anomaly detection and fraud scoring, and computer vision for image-based damage assessment in auto and property claims. This is where Exotica AI Solutions is building differentiated capabilities — helping insurance carriers move beyond basic bot automation into AI-driven workflows that improve continuously. No-code AI agents now make it possible for insurance ops teams to build and deploy these workflows without developer involvement.
You can also pair intelligent automation with AI chatbots and AI calling agents to create fully automated policyholder communication loops — from first notice of loss through settlement confirmation. Explore how this plays out in practice in our guide to Voice AI and chatbots as the new omni-channel standard.
Fraud Detection and Automated Document Validation
Automated document validation for fraud prevention in insurance is one of the highest-value applications in the industry. Insurance fraud costs US carriers an estimated $308 billion annually according to the Coalition Against Insurance Fraud. Manual fraud detection cannot scale against the volume and sophistication of modern fraudulent claims.
- Document authenticity checks — AI validates metadata, formatting, and field consistency to flag altered documents
- Cross-referencing — claims data automatically checked against provider records, billing history, and policy terms — powered by RAG-based knowledge retrieval
- Behavioral scoring — ML models assign fraud probability scores based on patterns invisible to human reviewers
- Real-time flagging — high-risk claims are escalated before payment is processed, not after
The Association of Certified Fraud Examiners (ACFE) reports that organizations using AI-driven anomaly detection recover significantly more in fraudulent claims than those relying on rule-based systems alone.
Developing an Insurance Automation Strategy
The benefit of developing an automation strategy for insurance is not just operational efficiency — it is building a compounding advantage. Each process you automate frees up human capacity for higher-value work, generates cleaner data for AI training, and reduces error rates across dependent downstream processes. Review our client case studies to see how this compounding effect plays out across insurance, healthcare, and financial services.
Recommended Automation Sequence:Phase 1 — Foundation: Claims intake, document classification, eligibility verification (highest volume, clearest ROI).
Phase 2 — Intelligence: Underwriting assistance, fraud scoring, and prior authorization workflows.
Phase 3 — Full orchestration: End-to-end policy lifecycle automation, customer communication automation, and predictive analytics.
For carriers exploring n8n workflow automation as the backbone of their automation stack, n8n’s self-hosted model offers data sovereignty that proprietary SaaS platforms cannot match — a critical consideration for regulated insurance environments.
What to Look for in Insurance Automation Software
When evaluating insurance automation software or a claims management platform, the criteria that matter most for mid-size and enterprise insurance organizations are:
| Criterion | What to Evaluate | Priority |
|---|---|---|
| Integration depth | Connects with existing PAS, CRM, and document tools without full system replacement | Critical |
| Configurability | Ops team can adjust rules and workflows without developer involvement for each change | Critical |
| AI capability | Goes beyond RPA to handle unstructured documents and variable exception inputs — powered by RAG and LLM integrations | High |
| Compliance support | Maintains audit trails and documentation required by NAIC and state and federal regulators | Critical |
| Scalability | Handles peak volume without degrading performance or requiring manual overflow handling | High |
| Reporting | Real-time dashboards on throughput, error rates, exception volume, and cost-per-claim | Medium |
Frequently Asked Questions
Insurance automation is not a future-state initiative anymore. The carriers, health plans, and agencies investing in it now are building structural advantages that will be very hard to close later. Whether you are starting with robotic process automation for a single claims workflow or implementing intelligent automation across your entire policy lifecycle, the compounding returns justify the move — and the window for early-mover advantage is still open.
Ready to build your insurance automation program? Talk to an Exotica AI Solutions expert today.

Mohit Thakur is an experienced Digital Marketing Expert, SEO Team Leader, and Content Writer with over 6 years of expertise in search engine optimization, content strategy, and digital growth. He specializes in research-driven SEO and crafting high-quality, compelling content that helps businesses improve their online visibility, organic traffic, and lead generation.
With hands-on experience across multiple industries, Mohit focuses on creating user-focused, well-researched content aligned with the latest Google algorithms and AI search trends. His approach combines technical SEO, content writing, content optimization, and data analysis to deliver consistent and measurable results.