What is insurance automation?
Insurance automation is the use of AI, robotic process automation (RPA) in insurance, and intelligent workflow technology to execute repetitive, rule-based tasks — automated claims processing, policy administration, eligibility verification, automated insurance underwriting, and compliance — without continuous human intervention. The result: faster operations, measurably lower costs, and insurance workflows that scale without adding headcount. Learn how AI is transforming the insurance industry in our companion guide.
Insurance Automation
If your team is still manually verifying eligibility, keying claims data between systems, or chasing document approvals by email — you’re burning margin that your competitors are not. Insurance automation has matured dramatically, and in 2026, the right insurance automation software is no longer a luxury reserved for Tier 1 carriers. Organizations of every size — MGAs, independent agencies, health systems, and regional carriers — are deploying AI tools for insurance automation to cut costs, reduce claim errors, and scale operations without growing headcount.
This guide cuts through the vendor noise and gives you an honest, experience-grounded breakdown of the most impactful insurance automation solutions available today — what they do well, which workflows they’re built for, and how to choose the right insurance process automation platform without wasting months on the wrong implementation.
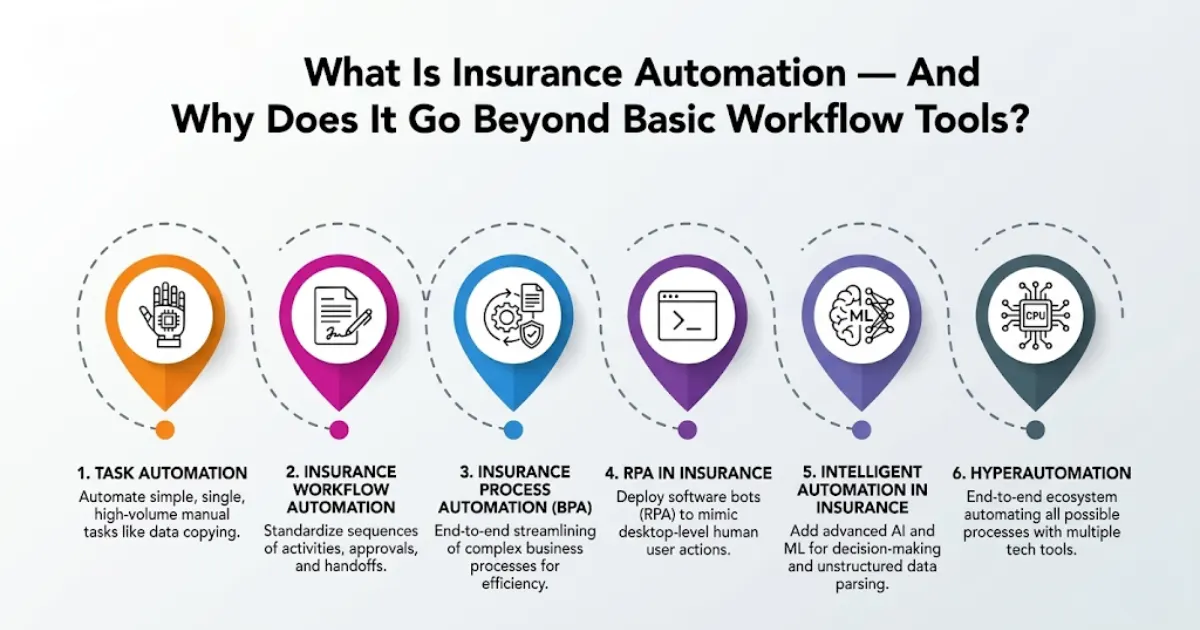
What Is Insurance Automation — And Why Does It Go Beyond Basic Workflow Tools?
Insurance automation refers to software platforms and AI-driven systems that orchestrate repetitive, rule-based insurance workflows across the full policy and claims lifecycle — from FNOL capture and automated claims adjudication to policy issuance, renewal management, and regulatory compliance filing. Automation in the insurance industry now encompasses everything from single-task bots to end-to-end intelligent process automation in insurance that learns and adapts over time.
The distinction from basic task automation matters. You’re not automating a single click. You’re automating an end-to-end insurance claims processing automation workflow, a multi-carrier eligibility verification sequence, or an automated insurance underwriting decisioning chain — with intelligent exception handling and audit trails built in. That’s what separates true insurance business process automation from basic integration scripts or single-step macro tools.
Modern insurance process automation platforms have deeply converged with AI — meaning they don’t just follow static rules anymore. They learn from claims patterns, surface fraud anomalies, and trigger underwriting actions based on predictive risk signals. That turns reactive insurance workflows into proactive, self-optimizing systems. For a broader look at how this convergence is reshaping the sector, see our analysis of
How AI is transforming the insurance industry.
| Automation type | What it handles | Best for | Example use cases |
|---|---|---|---|
| Task automation | Single-step, trigger-based actions | Small agencies, simple SaaS connections | New lead to CRM, policy renewal reminder emails |
| Insurance workflow automation | Multi-step, conditional sequences across systems | Mid-market agencies and MGAs | Eligibility check → benefits breakdown → denial alert |
| Insurance process automation (BPA) | End-to-end orchestration: humans, decisions, data | Regional carriers and enterprise departments | Full claims lifecycle from FNOL to payment |
| RPA in insurance | UI-level mimicry of human actions across legacy systems | Carriers with on-premise or legacy policy systems | Data re-entry between PMS and claims platforms; RPA in insurance claims |
| Intelligent automation in insurance | Adaptive, self-improving workflows with ML and NLP | Document-heavy, decision-intensive insurance processes | Automated underwriting, fraud scoring, intelligent document processing |
| Hyperautomation | Enterprise-wide: RPA + AI + process mining | Full digital transformation programs at Tier 1 carriers | Exotica AI custom stacks, UiPath, Pega |
Benefits of Automation in the Insurance Industry
The benefits of automation in the insurance industry are measurable, documented, and compounding. Organizations that have deployed automation in the insurance industry at scale consistently report outcomes across five dimensions: speed, cost, accuracy, compliance, and customer experience. Here’s what the data shows:
60–80%Reduction in standard insurance claims processing cycle time — from 8–12 days to 24–48 hours for straight-through claims.
95%+Reduction in manual automated insurance eligibility verification time — from 10–20 minutes per patient to under 30 seconds.
15–30%Reduction in fraudulent payouts through AI fraud scoring embedded in automated insurance claims workflows.
60–70%Faster per-transaction processing in insurance policy automation — new business issuance, endorsements, and renewals.
3–5×Faster lead response time from insurance agency marketing automation and AI-scored sales pipeline management.
40–60%Reduction in compliance preparation time through automation in insurance industry regulatory filing workflows.
Beyond the numbers, the strategic benefit of developing an automation strategy for insurance is compounding — each automated process generates cleaner data, which trains better AI models, which enables more sophisticated automation in the next cycle. Organizations that started automating insurance claims processing in 2023–2024 are now operating self-optimizing claims environments that continuously improve without additional implementation spend.
Why Insurance Organizations Are Searching for Automation Solutions Right Now
The demand for insurance automation software and intelligent automation in insurance has surged in 2026 — and the drivers are structural, not cyclical. Here’s what’s pushing real insurance business owners to prioritize automated insurance solutions:
- Labor costs keep climbing. Manual claims processing and eligibility verification are now among the most expensive per-transaction costs in operations. Insurance process automation is a core margin strategy, not an IT experiment.
- Claim volumes are rising faster than headcount can. Carriers and TPAs processing growing claim volumes need automated claims processing insurance workflows that scale without linear staff additions. According to McKinsey’s insurance AI research, automation can reduce claims processing costs by up to 30%.
- Compliance complexity is increasing. State-by-state regulatory requirements demand consistent, documented processes. Insurance workflow automation creates the audit trail that manual processes cannot. The National Association of Insurance Commissioners (NAIC) continues to expand model automation-related guidance.
- Customer expectations for speed have never been higher. Policyholders expect claims decisions in hours, not weeks. The carriers deploying automated insurance claims workflows are setting the new service benchmark your customers now expect from everyone.
- AI is now table stakes. Insurance organizations that spent 2023–2024 evaluating AI tools are in full deployment in 2026. Intelligent automation in insurance is already running in production at your competitors. Read how AI is reshaping every line of insurance business in detail.
- Cognitive automation is enabling decisions, not just tasks. The shift from rule-based automation insurance robots to cognitive automation in insurance — systems that handle unstructured data and ambiguous inputs — means the range of automatable processes has expanded dramatically into underwriting, complex claims, and fraud detection.
The Top Insurance Automation Use Cases Delivering ROI in 2026
Automated Claims Processing — The Fastest Payback in Insurance Automation
Automated claims processing is the single highest-ROI application of insurance automation. It covers the full insurance claims process automation lifecycle: FNOL intake, intelligent document processing for insurance claims, coverage verification, rules-based adjudication, fraud scoring, payment triggering, and claimant status communication — all without manual data entry for standard claims. Automating insurance claims processing compresses what used to be an 8–12 day cycle into 24–48 hours for straight-through cases.
Automated Insurance Verification — The Hidden Time Sink That Automation Eliminates
For medical practices, dental offices, physical therapy groups, and any healthcare-adjacent operation, automated insurance verification may be the single fastest-returning automation investment. Manual eligibility and benefits verification consumes 10–20 minutes per patient per visit. Automated insurance eligibility verification pulls real-time data from payer systems in under 30 seconds. Automating health insurance verification also enables overnight batch processing — checking tomorrow’s entire schedule against payer systems before the first patient arrives. For best automated dental insurance verification software options and healthcare-specific platforms, explore our full insurance automation resources.
Automated Insurance Underwriting — Faster Decisions, Better Risk Selection
Automated insurance underwriting uses AI and predictive analytics to evaluate risk, generate quotes, and make binding decisions — often in seconds for personal lines and standard commercial accounts. Automated underwriting in insurance relies on ML models trained on actuarial loss data that pull from credit bureaus, telematics feeds, claims history databases, and third-party enrichment sources to produce risk scores automatically. Automated life insurance underwriting is one of the fastest-growing applications, with straight-through processing now covering the majority of term life submissions at leading carriers. For a deeper look at AI-driven decisioning, read how AI is transforming insurance underwriting.
Insurance Document Automation — Processing Unstructured Data at Scale
Insurance document automation uses AI-powered intelligent document processing insurance (IDP) to automatically extract, classify, validate, and route data from the full spectrum of insurance documents — applications, policies, endorsements, medical records, repair estimates, certificates of insurance, legal correspondence, and adjuster notes — without manual data entry. Automated document processing insurance and automated document extraction in insurance eliminate the largest single source of downstream data entry errors in claims and policy admin. This is a core capability of enterprise insurance automation programs.
Insurance Policy Administration Automation — The Operational Backbone
Insurance policy automation solutions handle the full policy administration lifecycle — new business issuance, mid-term endorsements, renewals, billing, cancellations, reinstatements, and regulatory compliance filings — through rules-based automation and RPA bots that connect directly to your core policy management system without requiring system replacement. How insurance companies automate policy administration typically starts with the highest-volume transaction types — renewals and endorsements — before expanding to full lifecycle coverage. See how this fits into a full insurance industry automation strategy.
Insurance Agency Automation — Marketing, Sales & Client Lifecycle
For independent agencies and MGAs, insurance agency automation extends well beyond transactional processing. Insurance agency marketing automation and insurance sales automation use CRM integration, behavioral triggers, and AI scoring to deliver personalized renewal outreach, cross-sell offers, lead routing, and re-engagement campaigns — at exactly the right moment in the client lifecycle. Marketing automation for insurance agencies now includes AI-generated campaign content, behavioral segmentation, and pipeline scoring that was previously only accessible to enterprise carriers. This is one of the fastest-growing segments covered in our insurance industry solutions overview.
RPA in Insurance: Use Cases, Benefits, and How It Works
Robotic process automation in insurance (RPA) uses software bots to replicate the exact steps a human would take when interacting with existing software — logging into systems, navigating screens, copying and pasting data, filling forms, and generating reports — without any changes to the underlying infrastructure. This makes RPA in the insurance industry uniquely powerful for carriers with legacy systems that lack modern APIs.
The top robotic process automation insurance use cases in 2026 include:
- RPA in insurance claims — automated FNOL data capture, claims status updates, and payment processing triggers across legacy claims systems
- RPA in insurance underwriting — automated data pull from third-party enrichment sources, bureau reports, and telematics feeds into the underwriting workbench
- Robotic process automation insurance claims processing — straight-through processing of standard claims from intake to payment without adjuster touchpoints
- RPA in life insurance — automated policy issuance, beneficiary updates, and surrender value calculations in life and annuity administration
- RPA in insurance industry compliance — automated regulatory filing generation and submission to state departments of insurance
- Insurance robotic process automation for eligibility — automated batch eligibility checks against payer systems at scale
The distinction between RPA automation insurance and broader intelligent automation insurance is important. Pure RPA follows fixed rules and breaks when the underlying UI changes. RPA and AI in insurance combined — sometimes called intelligent RPA or attended automation — uses AI to handle exceptions, read unstructured inputs, and self-heal when screen interfaces shift. Leading platforms like UiPath and Pega now ship both capabilities in a unified platform.
For organizations evaluating robotic process automation in insurance industry deployments, the RPA use cases in insurance that deliver the fastest payback are those where: (1) the process is high-volume, (2) the steps are perfectly consistent, and (3) the data sources are digital rather than handwritten. Start there — then expand to AI-enhanced automation as your bot estate matures.
Intelligent Process Automation in Insurance: Beyond RPA
Intelligent process automation in insurance (IPA) combines RPA with AI capabilities — machine learning, natural language processing, computer vision, and intelligent document processing — to automate processes that are too complex, too variable, or too unstructured for traditional RPA alone. Where RPA automates the steps, intelligent automation insurance automates the decisions.
The key intelligent automation in insurance capabilities that separate IPA from basic RPA are:
- Intelligent document processing insurance — AI that reads, classifies, and extracts data from handwritten notes, scanned EOBs, medical records, and non-standard document formats that OCR alone cannot handle
- Cognitive automation in insurance — systems that understand the context of a claim or application, not just the data fields, enabling exception handling that previously required human judgment
- Predictive analytics in underwriting — ML models that score risk from structured and unstructured inputs, enabling automated insurance underwriting systems that improve their accuracy over time
- AI platforms for automating insurance support services — conversational AI and knowledge retrieval systems that handle policyholder inquiries, claims status requests, and coverage questions without agent involvement
- Anomaly detection — real-time fraud scoring embedded in automated insurance claims processing that flags suspicious patterns before payment, not during post-payment audit
The how health insurance companies use automation to improve efficiency narrative has shifted from “we use RPA for data entry” to “our claims environment learns from every adjudication decision and applies those learnings to the next 10,000 claims automatically.” That shift — from mechanical automation to intelligent automation for policy servicing and claims — is what defines the leading carriers in 2026. Learn more about how intelligent automation is transforming insurance operations.
Ready to identify which insurance workflows are ready to automate first? Our team has delivered measurable ROI for carriers, MGAs, and healthcare organizations across every use case in this guide.
Quick Comparison: Insurance Automation by Use Case
| Use case | Best for | AI capability | Implementation complexity | Typical ROI timeline |
|---|---|---|---|---|
| Automated claims processing | Carriers, TPAs, health insurers | Advanced (fraud ML, IDP) | Medium — 3–6 months | 6–12 months |
| Insurance verification automation | Medical/dental practices | Strong (real-time payer API) | Low — days to weeks | 30–90 days |
| Automated underwriting | Personal lines, small commercial, life | Advanced (predictive ML) | High — 6–12 months | 12–18 months |
| Document automation (IDP) | Any high-document-volume operation | Advanced (NLP, OCR, CV) | Medium — 2–4 months | 3–9 months |
| RPA in insurance claims | Carriers with legacy systems | Moderate (rules + attended AI) | Low-Medium — 1–3 months | 2–6 months |
| Policy administration | Carriers, MGAs | Strong (RPA + rules engine) | Medium — 3–6 months | 6–12 months |
| Agency marketing automation | Independent agencies | Strong (CRM AI scoring) | Low — weeks | 30–60 days |
How to Choose the Right Insurance Automation Solution
Choosing the wrong insurance process automation platform costs more than money — it costs six to eighteen months of failed implementation and organizational confidence. Here’s the decision framework experienced operators use when evaluating insurance automation software:
-
Audit your highest-volume, most repetitive workflows first. Don’t start with vendor demos. Start with a process audit. Document where manual handoffs happen, where errors occur, and where backlogs form. The best AI tools for insurance automation won’t deliver value if you’re automating a broken process. This is the foundation of any sound insurance automation strategy. Our insurance automation readiness guide walks through how to identify your best starting point.
-
Assess your current technology environment. What is your core policy management system? Do you have legacy on-premise platforms that need robotic process automation in insurance to bridge? What’s your team’s technical capacity? Your answers immediately eliminate half the solutions on the market — and protect you from scoping a platform you cannot operationally support. AMS with automation features for insurance is the right starting point for many independent agencies.
-
Define your scale and compliance requirements. A dental practice automating eligibility verification needs a fundamentally different platform than a regional carrier running end-to-end insurance claims processing automation under state insurance department oversight. Volume, regulatory requirements, and exception-handling complexity should drive your selection — not feature comparison spreadsheets. The NAIC publishes current state-by-state compliance guidelines worth reviewing before any platform commitment.
-
Evaluate total cost of ownership — not just license fees. Many software for automating insurance claims processing platforms appear affordable at entry level and become expensive at production scale. Factor in implementation time, staff training, ongoing maintenance, integration development, and insurance automation consulting costs if your team lacks in-house implementation expertise.
-
Pilot before you commit. Every credible vendor will support a proof of concept on a real workflow. Run one end-to-end — FNOL to payment, or eligibility check to benefit display — before signing an annual contract. This surfaces integration gaps and exception-handling failures that vendor demos always hide. Talk to our team about structured pilots designed for insurance-specific environments.
AI-Powered Insurance Automation: What’s Actually New in 2026
The most significant shift across all insurance automation software in 2026 is the deep convergence with generative AI and large language models. Every serious insurance process automation platform has added AI layers — but the real change is in how that AI is being operationalized. For a comprehensive breakdown, read our full guide on how AI is transforming the insurance industry:
- Intelligent document processing for insurance claims — top platforms now handle fully unstructured inputs — handwritten notes, scanned EOBs, voice-to-text adjuster recordings — without manual extraction template setup. This is the backbone of modern RAG-based knowledge retrieval inside insurance workflows.
- AI-assisted workflow design — the best insurance workflow automation platforms in 2026 let operations teams describe a claims or underwriting process in plain language and auto-generate the automation logic — no developer required for configuration. Gartner’s hyperautomation framework provides useful context for how this capability is evolving.
- Anomaly detection and compliance monitoring — AI compliance tools flag claim anomalies, document inconsistencies, and coverage mismatches before they become payment errors or regulatory exposure. Critical for health insurance claims automation and financial reconciliation workflows.
- AI insurance sales automation — leading platforms now trigger personalized renewal sequences, score cross-sell opportunities, and update CRM records without producer intervention — compressing the agency sales cycle without adding staff. AI insurance sales automation benefits include measurable improvements in renewal retention and pipeline conversion.
- Automated insurance marketing — AI-powered tools generate, personalize, and schedule client communication campaigns based on behavioral signals and policy lifecycle events, entirely within the insurance agency automation stack.
- Conversational process triggers — insurance automation can now be initiated through AI chatbot inputs or voice commands — not just form submissions — reflecting the rise of self-service portals and omnichannel policyholder experiences.
- Custom AI automation stacks for insurers — carriers and MGAs building automation outside standard SaaS platforms are increasingly deploying n8n workflow automation for self-hosted, extensible claims and policy pipeline orchestration. Automation in life insurance specifically has seen rapid adoption of these custom stacks for illustration, policy issuance, and beneficiary management.
Firms like Exotica AI Solutions are helping mid-market carriers, MGAs, and healthcare organizations implement these AI-powered insurance automation solutions — bridging the gap between platform selection and production-scale deployment with measurable, documented ROI.
Common Mistakes Insurance Organizations Make When Implementing Automation
- Automating without process standardization first. If five adjusters handle the same claim type five different ways, your platform locks in inconsistency, not efficiency. Standardize your claims or underwriting workflow first — then automate it. Our insurance automation readiness overview outlines where most organizations should begin.
- Underestimating change management. Underwriters and claims staff resist insurance automation tools when deployment feels like a job threat rather than a relief from tedious work. Communication and redeployment planning matter as much as the technology. Harvard Business Review’s change management research is useful context here.
- Over-engineering the first workflow. Start with high-volume, low-complexity processes — automated eligibility checks or certificate of insurance generation. Quick wins build organizational confidence and surface real-world edge cases safely before you tackle end-to-end insurance claims process automation.
- Ignoring exception handling. Every automated insurance workflow will hit an edge case — an unusual coverage combination, a missing document, a multi-party claim. Build exception routes and human escalation paths from day one, or your automation insurance claims solution creates a backlog instead of clearing one.
- Not measuring baseline performance. You cannot prove ROI on insurance busines33322n,,llll process automation if you didn’t document how long the manual process took. Measure cycle time, error rate, and headcount cost before you automate — not after. Read more on building a data-driven insurance automation business case.
- Treating RPA as the end state. Robotic process automation insurance is a starting point, not a destination. Organizations that deploy RPA and stop there miss the compounding returns that come from layering AI on top — intelligent document processing, predictive fraud scoring, and adaptive underwriting decisioning.
Insurance Automation by Function: Where the ROI Is Highest
| Insurance function | High-ROI automation use cases | Typical efficiency gain |
|---|---|---|
| Claims | FNOL intake, intelligent document processing insurance claims, coverage verification, adjudication, fraud scoring, payment triggering, claimant communication | 60–80% reduction in standard insurance claims processing cycle time |
| Underwriting | Risk scoring, straight-through processing, automated data entry for insurance claims, third-party enrichment, quote generation | 50–70% reduction in quote turnaround for personal lines |
| Policy Administration | New business issuance, endorsements, renewals, billing, cancellations, compliance filings | 60–70% reduction in per-transaction processing time |
| Eligibility & Benefits Verification | Real-time and batch automated insurance eligibility checks, benefits breakdown, prior auth tracking, denial prevention | 95%+ reduction in manual verification time per patient |
| Agency Sales & Marketing | Lead scoring and routing, renewal outreach sequences, cross-sell triggers, CRM hygiene, insurance agency marketing automation | 3–5× faster lead response; 10–20% improvement in renewal retention |
| Compliance & Reporting | Regulatory filing automation, audit trail generation, exception reporting, carrier appointment tracking | 40–60% reduction in compliance preparation time |
| Life Insurance | Automation in life insurance — illustration, policy issuance, beneficiary updates, surrender calculations, automated life insurance underwriting | 50–65% reduction in new business processing time |
Frequently Asked Questions
Final Verdict: Which Insurance Automation Solution Should You Choose?
There is no single best insurance automation platform — only the right insurance process automation solution for your specific organization, workflow volume, and regulatory environment. Here’s the short version:
Small agency / startup: Start with insurance agency marketing automation and automated eligibility verification — the fastest ROI with the lowest implementation barrier.
See agency-specific automation options
Medical or dental practice: Automated insurance verification and health insurance claims automation — eliminates the #1 front-desk time drain and cuts denial rates immediately. Best automated dental insurance verification software options are covered in our full industry guide.
MGA or regional carrier: Insurance document automation (IDP) + policy administration automation — eliminate manual data entry across your highest-volume transaction types first.
Explore MGA automation solutions
High-volume P&C or health carrier: End-to-end automated claims processing with integrated fraud scoring — the largest single ROI opportunity in carrier operations. Combine with RPA in insurance claims for legacy system connectivity.
Life insurance carrier: Automation in life insurance — automated life insurance underwriting, policy issuance, beneficiary management, and illustration workflow automation deliver the fastest payback for life and annuity operations.
Regulated carrier with complex decisioning: Automated underwriting with AI-powered adaptive models — the gold standard for carriers managing risk selection at scale under regulatory oversight. Read how AI is reshaping insurance decisioning in our detailed guide.
The insurance organizations winning in 2026 are not the ones with the most sophisticated automation insurance tools. They’re the ones that selected the right insurance automation solution, implemented it correctly around standardized processes, and continuously optimized their workflows based on real operational data. The benefits of automation in the insurance industry are real and measurable — but they require disciplined implementation, not just platform selection. Working with experienced insurance automation experts — like Exotica AI Solutions — compresses that learning curve significantly and helps you avoid the costly implementation mistakes that derail most insurance automation projects before they deliver measurable value.
Start with one workflow. Automate it well. Then scale.
Talk to the Exotica AI Solutions team today.

Mohit Thakur is an experienced Digital Marketing Expert, SEO Team Leader, and Content Writer with over 6 years of expertise in search engine optimization, content strategy, and digital growth. He specializes in research-driven SEO and crafting high-quality, compelling content that helps businesses improve their online visibility, organic traffic, and lead generation.
With hands-on experience across multiple industries, Mohit focuses on creating user-focused, well-researched content aligned with the latest Google algorithms and AI search trends. His approach combines technical SEO, content writing, content optimization, and data analysis to deliver consistent and measurable results.